The Brain Science Behind PANS & PANDAS
A neuroscience-informed look at why PANS and PANDAS produce sudden psychiatric symptoms, and why understanding the biology changes how we respond.
Understanding PANS & PANDAS
Neuroimmune disorders affecting the brain.
PANS and PANDAS are conditions in which the immune system attacks the brain, causing sudden and severe symptoms. Think of the brain as “on fire”: a neurological storm, not intentional behavior. Symptoms can appear quickly and intensely, often within days.
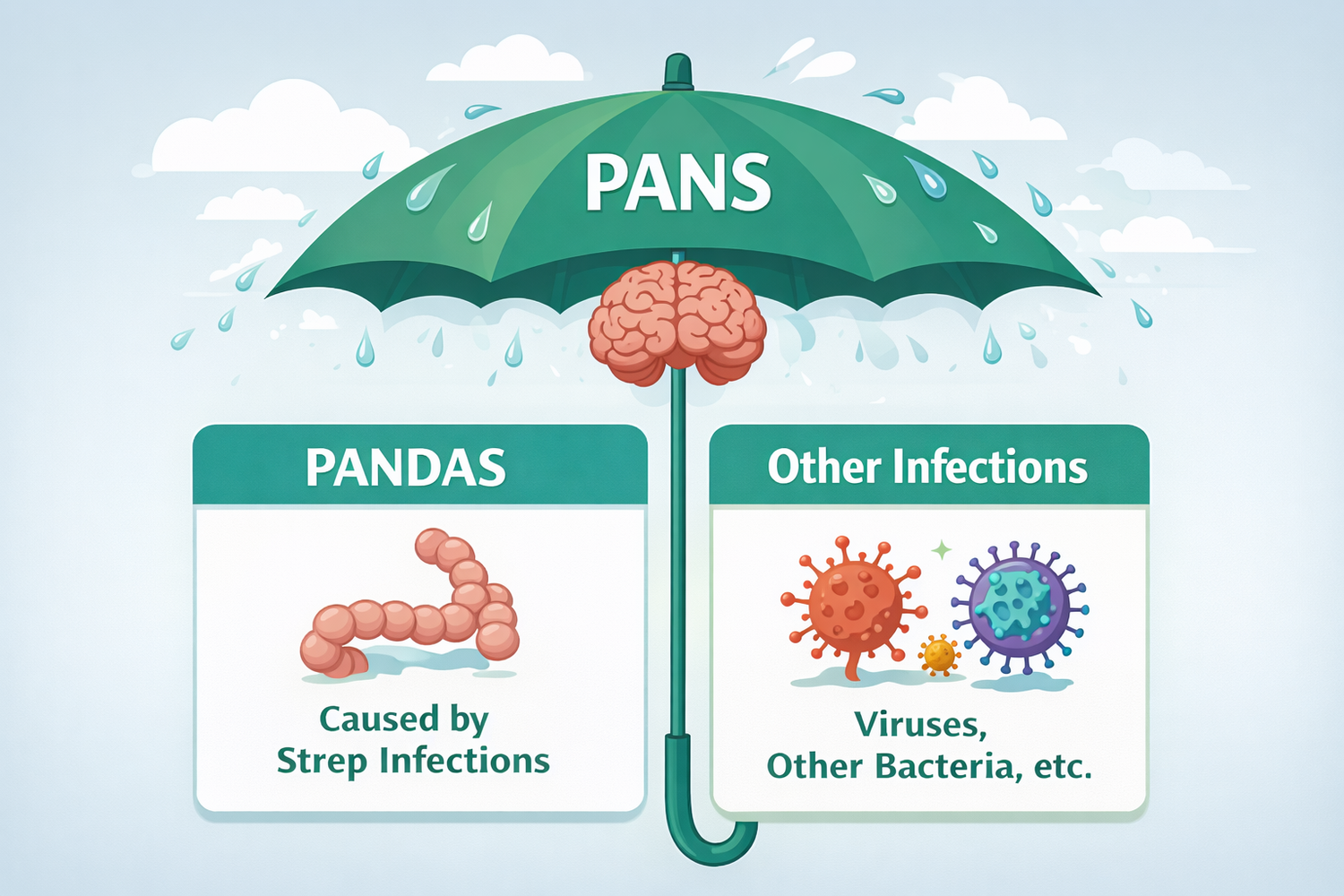
PANS is the Umbrella
PANDAS sits underneath it.
PANS (Pediatric Acute-onset Neuropsychiatric Syndrome) is the broader category. It covers any sudden neuropsychiatric onset triggered by an immune response to viruses and infections, including Mycoplasma pneumoniae, Lyme, influenza, COVID-19, and other bacterial illnesses.
PANDAS (Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections) is a specific subset, the strep-triggered slice of PANS.
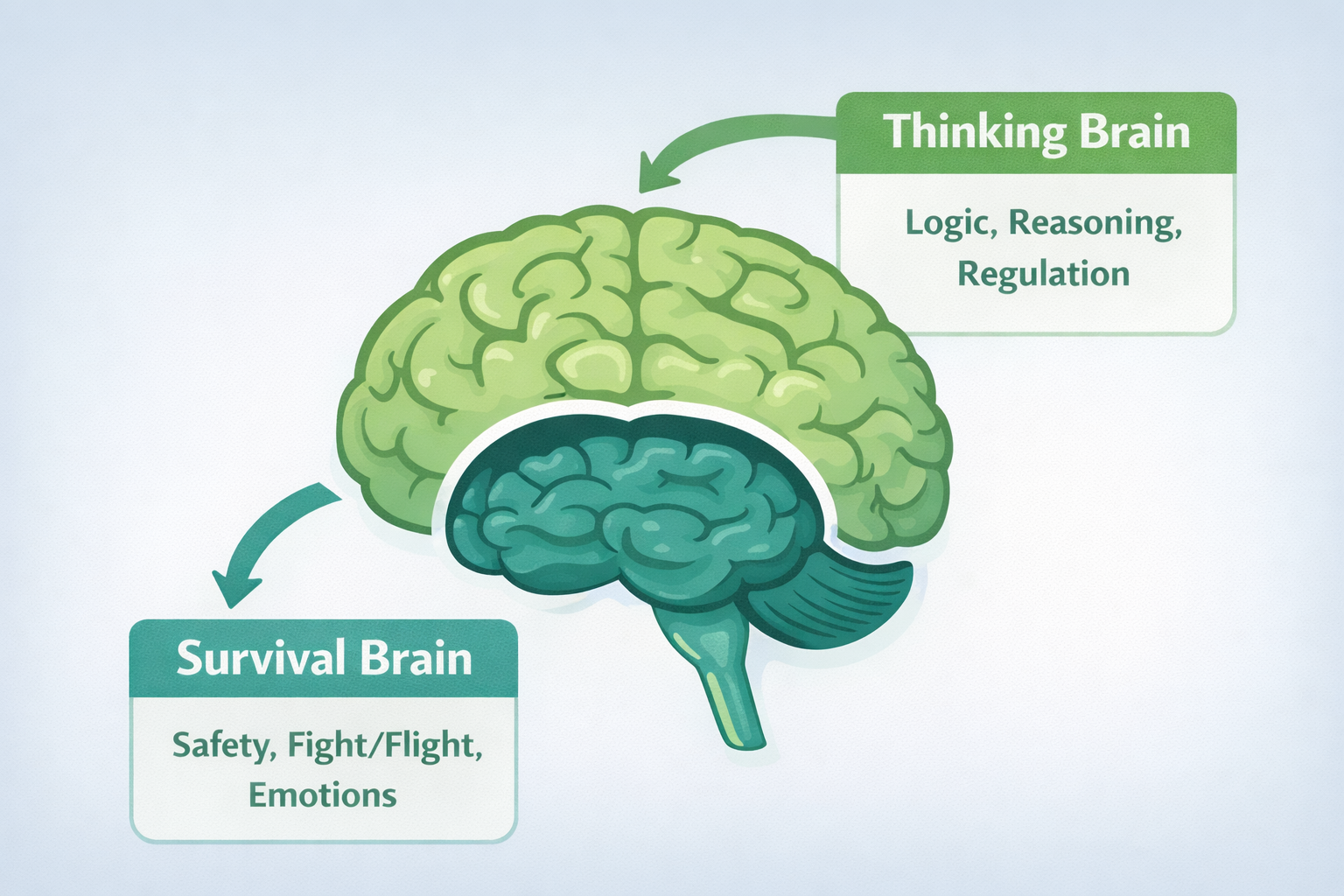
The Brain Works in Layers
Lower regions keep you alive. Higher regions help you reason.
The brain is not a single system. It is organized in layers that developed over time. Lower brain regions are focused on survival. Higher brain regions are focused on learning and regulation. When the brain feels safe, higher regions guide behavior. When the brain feels threatened, or is inflamed, lower regions take control.
PANS/PANDAS create exactly the conditions that tip the system downward: inflammation, immune activation, pain, exhaustion, and disrupted sleep all signal "threat" to the brain, even when no external threat is present.
That tipping is why a child in flare cannot simply "talk themselves down" or use coping skills they had a month ago. The system that would allow a child to coping is completely offline.
⬆ Survival (Bottom-Up) System
Brainstem · Amygdala · Basal Ganglia
Functions:
- Detect threat
- Drive fight, flight, freeze
- Control habits and automatic responses (keeping you alive without thinking about it)
This system runs:
- Respiration: regulating your breathing rhythm.
- Circulation: controlling heart rate and blood pressure.
- Digestion: managing gut activity and food processing.
- Thermoregulation: maintaining your core body temperature.
- Sleep-wake cycles: regulating arousal and sleep.
- Reflexes: involuntary responses like sneezing, coughing, vomiting, and swallowing.
- Balance & posture: coordinating movements and maintaining stability.
- Sensory processing: relaying visual, auditory, touch, taste, and smell signals.
- Hormonal regulation: the hypothalamus manages thirst, appetite, and stress responses.
⭐️ Its job is to: detect danger, react quickly, keep the body alive.
❗ It is fast, automatic, and emotional, and it does not reason.
⬇ Thinking / Learning (Top-Down) Systems
Prefrontal Cortex · Higher Cortical Networks
Functions:
- Reasoning (think logically)
- Emotional regulation
- Flexibility (reflect and problem-solve)
- Perspective-taking
- Control impulses
⭐️ This system works only when the brain feels safe.
It is slower than the survival system, by design. Reasoning requires time, energy, and the safety to pause. When the body is fighting infection or the immune system is activated, the brain’s first priority is not nuance; it’s protection. The thinking system goes quiet.
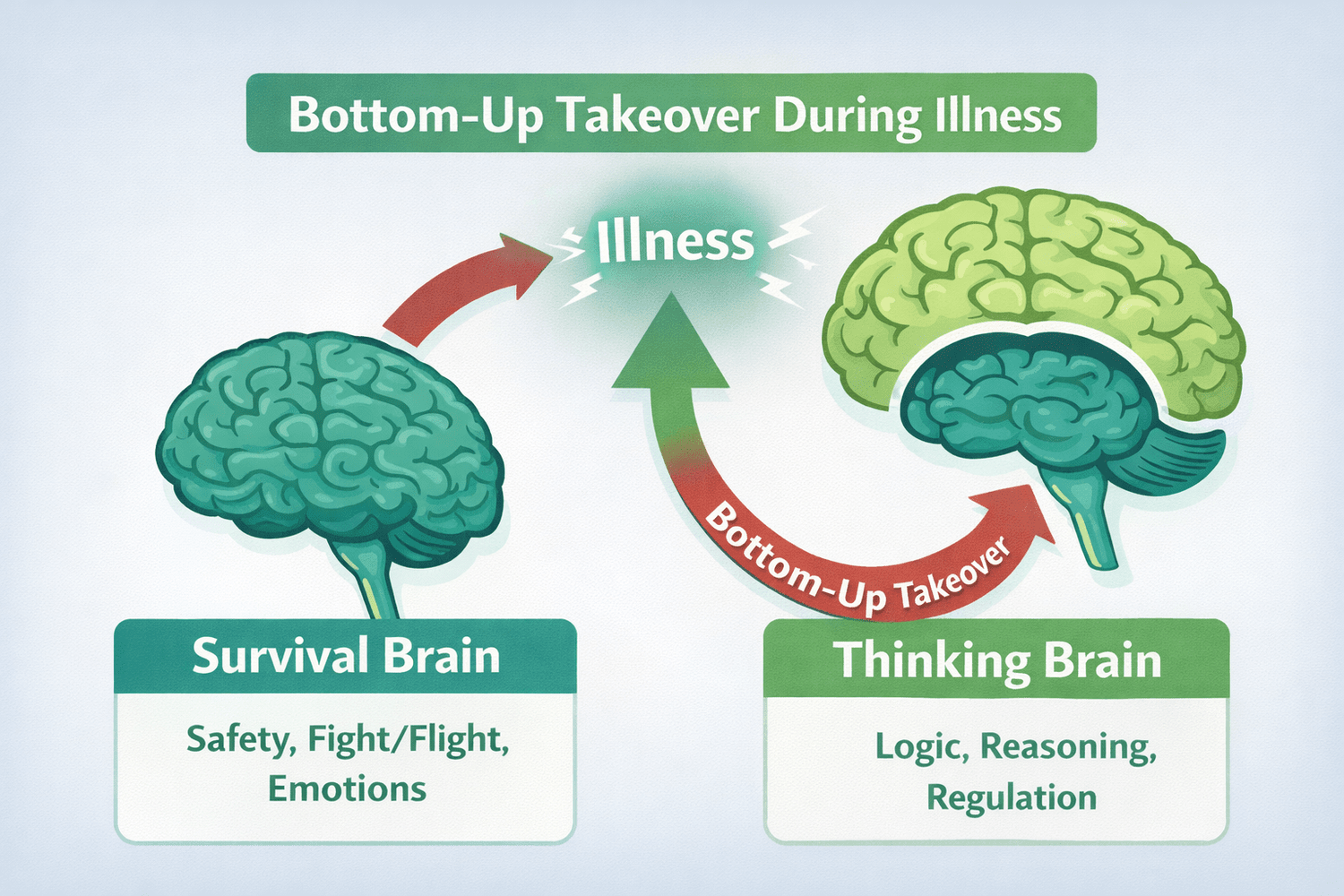
Bottom-Up Takeover
In PANS/PANDAS, inflammation pushes control downward.
Survival systems dominate. Thinking systems lose influence. This is called bottom-up takeover, the neurological reality behind the behaviors families describe as “Jekyll and Hyde.”
Why Parents Feel Like “Nothing Works”
Most parenting strategies require an online learning brain.
Most parenting strategies rely on:
- Verbal instruction
- Cause and effect
- Emotional regulation
These require an online learning brain. During illness, the child’s brain is operating from a survival platform, making traditional strategies ineffective or even escalating.
Parent Reframe
Your child cannot “use logic” when the survival brain is in charge. Your child is not refusing to think, their brain is protecting them. Remember: the brain’s priority is to keep us alive, not to keep us happy.
The Immune-to-Brain Pathway
How an infection becomes a neurological event.
Researchers have proposed several overlapping mechanisms that connect an immune event in the body to a neurological event in the brain. Most cases likely involve more than one.
1The Mistaken Identity
Strep and certain other germs wear proteins on their surface that look a lot like proteins on the child’s own brain cells, especially in the part of the brain that governs habits, movement, and the on/off switch for obsessive thoughts (the basal ganglia). When the immune system makes weapons (antibodies) to fight the infection, those weapons can mistake the child’s own brain cells for the germ, and attack by accident.
2The Wrong-Address Antibodies
Research led by Dr. Madeleine Cunningham has identified specific antibodies that bind to brain cells and switch on a molecular alarm called CaMKII. When that alarm is firing too much, the way brain cells communicate with each other changes, and so does behavior. Higher alarm activity tracks with more severe psychiatric symptoms.
3The Brain’s Gate Opens
The brain has a security gate called the blood-brain barrier that normally keeps most immune cells and inflammation out. When the body is fighting an infection, that gate can loosen, and antibodies and inflammatory signals that should never reach the brain get through.
4Chemical Alarms in the Brain
Infection releases chemical alarm signals called cytokines. Those signals tell the brain’s own immune cells (the microglia) to switch into “fight mode.” Active microglia change the balance of brain chemistry and disrupt the circuits that govern mood, anxiety, and behavior.
Why the Basal Ganglia Matter
The brain region at the center of both childhood OCD and immune-mediated OCD.
The basal ganglia are a cluster of deep brain structures that govern habit formation, motor control, the start/stop of movements, and the gating of obsessive thoughts. They are also one of the regions most consistently implicated in OCD, tics, and Tourette syndrome.
Neuroimaging studies of children with PANDAS have shown increased basal ganglia volume during flares, a measurable marker of inflammation that often normalizes as the child recovers. This is why the same brain region involved in typical childhood OCD becomes the central player in immune-mediated OCD as well.
Why It Looks Psychiatric
Same brain regions, very different cause.
PANS/PANDAS affect brain regions involved in:
…so the symptoms often look psychiatric on the surface: OCD, anxiety, rage, regression (bedwetting, regression in academic skills, regression in handwriting), eating restriction or avoidance of specific foods or textures.
Next Step
Want help making sense of your child’s picture?
A discovery call is a conversation, not a commitment. We’ll listen to what your family is navigating and point you toward what to do next.
The Beta Program is a non-medical mental health practice. Information on this page is educational and does not constitute medical advice, diagnosis, or treatment.